Hypersensitivity
- Hypersensitivity is defined as injurious consequences in the sensitized host, following contact with specific antigen.
- Hypersensitivity is defined as an exaggerated or inappropriate state of normal immune response with onset of adverse effects on the body.
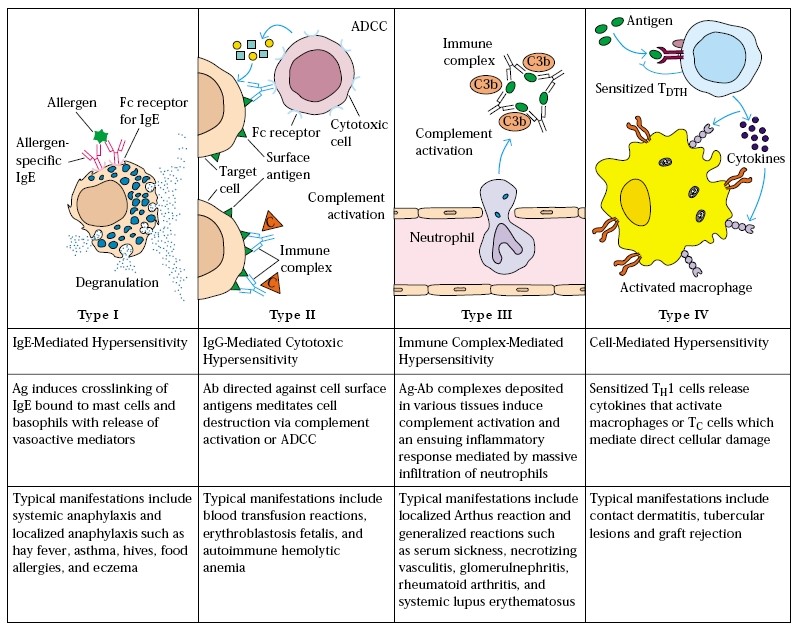
- Coombs & Gell classifed hypersensitivity reactions into four types based on the different mechanisms of pathogenesis as TypeI, II, III & type IV.
- Depending upon the rapidity, duration, and type of the immune response, 4 types of hypersensitivity reactions are grouped into immediate and delayed type.
Difference between Immediate and Delayed Hypersensitivity
|
Immediate hypersensitivity
|
Delayed hypersensitivity
|
|
Appears & recedes rapidly
|
Appears slowly & lasts longer
|
|
Induced by haptens or antigens by any route
|
Antigen or hapten intradermally or with Freud’s adjuvant or by skin contact
|
|
Circulating antibodies present are responsible
|
Circulating antibodies may be absent & not responsible for reaction; ‘cell mediated’ reaction
|
|
Passive transfer possible with serum
|
Cannot be transferred with serum; but possible with T cells or transfer factor.
|
|
Desensitisation easy, but short-lived
|
Difficult, but long-lasting
|
Types of hypersensitivity & their features
|
Type of reaction
|
Clinical syndrome
|
Time required for manifestation
|
Mediators
|
|
Type I: IgE type
|
- Anaphylaxis
- Atopy
|
Minutes
|
IgE:histamine & other pharmacological agents
|
|
Type II: cytolytic & cytotoxic
|
Antibody mediated damage-thrombocytopenia-agranulocytosis, hemolytic anemia, etc.
|
Variable: hours to days
|
IgG: IgM, C
|
|
Type III: Immune complex
|
- Arthus reaction
- Serum sickness
|
Variable: hours to days
|
IgG: IgM, C
|
|
Type IV: delayed hypersensitivity
|
- Tuberculin
- Contact dermatitis
|
Hours to days
|
T cells; lymphokines; macrophages
|
Type I Hypersensitivity reaction/ IgE dependent
- These occur in two forms: the acute, potentially fatal, system form called anaphylaxis & the chronic or recurrent, non fatal, typically localised form called atopy.
Anaphylaxis:
- This is the classical immediate hypersensitivity reaction.
- Antigens and hapten can induce anaphylaxis. There should be atleast 2-3 weeks of interval between the sensitising dose & the shocking dose.
Atopy:
- The term atopy refer to naturally occurring familial hypersensitivities of human beings, typified by hay fever & asthma.
- The antigens involved in atopy are characteristically inhalants (for example, pollen, house dust) or ingestants (for examples, eggs, milk).
Mechanism of Type I HSN
- a. Sensitization phase
Priming dose of antigen (allergen)->processed by APC->antigen peptide presented to T cell->Th2->secretes IL4->Acts on B cell->IgE produced-> Mast cell coated with IgE (Fc).
- b. Effector phase
Shocking dose->IgE (Fab) binds to antigen-> Mast cell degranulation.
- Tissues or organs predominantly involved are known as target tissues or shock organs.
Type II Hypersensitivity reaction/Cytolytic & cytotoxic
- Type II or cytotoxic reaction is defined as reactions by humoral antibodies (IgG, rarely by IgM) that attack cell surface antigens on the specific cells & tissues & cause lysis of target cells.
- Type II reaction appears generally within 15-30 mins after exposure to antigen.
- In general, type II reactions have participation by complement system, tissue macrophages, platelets, natural killer cells, neutrophils & eosinophils while main antibodies are IgG and IgM.
- Type II hypersensitivity is tissue-specific & reaction occurs after antibodies bind to tissue specific antigens, most often on blood cells.
- Example of Type II hypersensitivity
- Erythroblastosis fetalis
- Good Pasteur syndrome
- Grave’s disease
- Myasthenia gravis.
Type III Hypersensitivity reaction/ Immune complex diseases
- It results from deposition of antigen-antibody complexes on tissues, which is followed by activation of the complement system and inflammatory reaction, resulting in cell injury.
- The onset of type III reaction takes place about 6 hours after exposure to the antigen.
- Type III reaction is not tissue specific & occurs when antigen-antibody complexes fail to get removed by the body’s immune system.
- Clinical Syndrome: (a) Arthus reaction (b) Serum sickness.
- There can be 3 possible etiologic factors precipitating type III reaction:
- Persistence of low-grade microbial infection.
- Extrinsic environmental antigen.
- Autoimmune process.
Examples:
- Hypersensitivity Pneumonitis (Farmer’s lung)
- Post streptococcal glomerulonephritis.
- Nephrotic syndrome in Plasmodium malariae.
- Katamaya fever in schistosomiasis.
- Connective tissue disorder-SLE, Rheumatoid Arthritis.
Type IV/ delayed or cell mediated hypersensitivity
- Type IV reaction is tissue injury by cell mediated immune response without formation of antibodies but is instead a slow & prolonged response of specifically sensitised T lymphocytes (CD4 &CD8 T cells).
- The reaction occurs about 24 hours after exposure to antigen & the effect is prolonged which may last up to 14
Examples:
- Tuberculin test-Mantoux/Heaf
- Lepromin test
- Montenegro test (Leishmania)
- Multiple sclerosis
- Chronic transplant rejection
- Graft-versus host disease
|
Deficiency of complement
|
Syndrome associated
|
|
C1 Esterase inhibitor
|
Hereditary angioneurotic oedema
|
|
Early components of classical pathway (C1, C2, C4)
|
SLE & other collagen vascular disease
Pyogenic infection
|
|
C3 and its regulatory protein
|
Severe recurrent pyogenic infection
|
|
Complement C5-9 (membrane attack complex)
|
Gram –ve diplococci (Neisseria), Toxoplasma
|
|
D, I
|
Pyogenic infections
|
|
Properdin
|
Neisseria infections
|
|
H
|
Hemolytic uremic syndrome
|