IMMUNOLOGY
Latin-immunis meaning free from burden, freedom from disease.
It is defined as the state of resistance or insusceptibility exhibited by the host to toxic molecules, microorganism and foreign cells.
Immunity can be broadly classified in to two types:
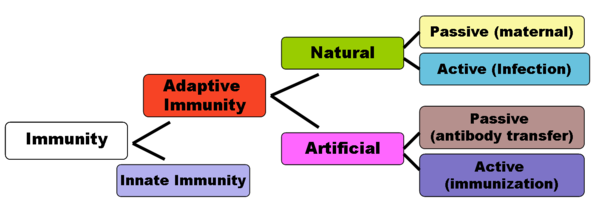
Types of Innate immunity:
Species immunity
Racial immunity
Individual Immunity
Factors affecting Innate Immunity
AGE: The two extremes of life, i.e. foetus (immune apparatus is immature) and old person (immune response is waning) carry high susceptibility of infectious diseases.
The foetus in utero is normally protected by placental barrier from maternal infection. Certain pathogens, e.g. Rubella, Cytomegalovirus, Toxoplasma gondii cross the placental barrier leading to congenital malformation.
Hormonal influences: Endocrine disorders like diabetes mellitus are associated with increased risk of infections.The increased risk may be related to increased levels of carbohydrate intissues.
Corticosteroids depress the individuals resistance by its anti inflammatory and anti phagocytic effects. The effect of stress in increasing susceptibility to infections may be due to release of steroids.
NUTRITION: In general, both humoral and cell mediated immune process are reduced when there is malnutrition and thus predisposes host various infections like bacterial septicaemia, tuberculosis, herpers virus infection, measles, candidiasis.
Innate immunity: mechanisms
Phagocytosis is the process of endocytosis in which the cell engulfs the foreign particles in a phagocytic vacuole and kills or inactivates them. A wide range of phagocytic cells are involved in the process such as blood monocytes, tissue macrophages, dendritic cells, nutrophils etc.
Steps of phagocytosis:
Natural Killer (NK) cells: They are a class of lymphocytes that kill virus infected cells and tumor cells.
Mast cells: They are present lining the respiratory & other mucosa.
They are activated by microbial products binding to toll-like receptors or by IgE antibody dependent mechanism, following which they release abundant cytoplasmic granules rich in histamine, prostaglandins & cytokines that initiate inflammation &proteolytic enzymes that results in killing of bacteria.
Dendritic cells: they respond to microbe by producing numerous cytokines that initiate inflammation. They also serve as vehicle in transporting the antigens from the skin and mucosal sites to lymph nodes where they present antigens to T cells.
It is also an important physiological barrier. Fever results in the increase body temperature which enhances the rate of synthesis of leukocytes and inhibit the further amplification of the pathogens.
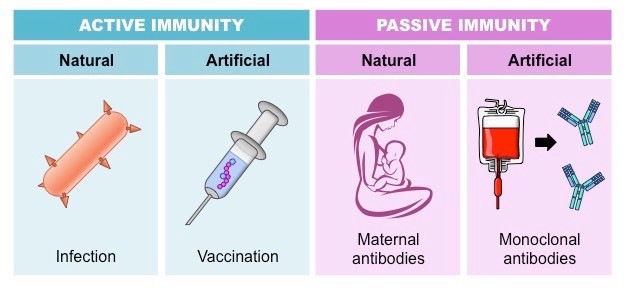
Acquired immunity
Acquired (adaptive): resistance acquired by an individual during life.
Active immunity
It is the immunity acquired by the individual by the inoculation of antigen or by the infectious microbes. In this type, the host immune response is provoked (activated) by the microbes or their components (Antigen).
Adaptive immunity: mechanisms
Main components of innate and acquired immunity that contribute to humoral and cell-mediated immunity. Table below compares the differences between these two types of immunity.
|
Immunity type |
Humoral immunity |
Cell-mediated immunity |
|
Innate immunity |
Complement neutrophils |
Macrophages Natural killer cells |
|
Acquired immunity |
B-cells Plasma cells |
Helper T cells Cytototoxic cells |
Cell-mediated immune response
T-cell
T-cell goes into effectors cells stage that is able to kill infected cells
2 types
Types of immune response in active immunity vary depending upon the microbial exposure that occurs the first time (Primary immune response) and subsequent time (Secondary immune response).
Primary response
Secondary response
Example - cytotoxic reactions against intracellular parasites, delayed hypersensitivity (e.g., Tuberculin test) and allograft rejection
B cells
Difference between active and passive immunity
|
Active immunity |
Passive immunity |
|
Produced actively by host's immune system. |
Received passively. No active host participation. |
|
Induced by infection or by immunogens. |
Readymade antibody transferred. |
|
Durable effective protection. |
Transient, less effective. |
|
Immunity effective only after lag period. |
Immediate immunity. |
|
Immunological memory present. |
No memory. |
|
Booster effect on subsequent dose. |
Subsequent dose less effective. |
|
Negative phase may occur.> |
No negative phase. |
|
Not applicable in the immunodeficient. |
Applicable in the immunodeficient. |
A simple method of testing immunity is to relate its level to some convenient indicator, such as demonstration of the specific antibody. The antibodies may be demonstrated by a variety of techniques such as agglutination, precipitation, complement fixation, hemagglutination inhibition, neutralisation, enzymelinked immunosorbent assay (ELISA). Where protection is associated with cell mediated immunity, skin tests for delayed hypersensitivity and invitro tests are used as an indicator of immunity
In poliomyelitis systemic immunity provided by active immunisation with the killed vaccine neutralises the virus when it enters the bloodstream, but it does not prevent multiplication of virus at the site of entry (the gut mucosa) and its fecal shedding. This is achieved by local intestinal immunity either acquired by infection or immunisation with live oral vaccine. A special class of immunoglobulins(IgA)forms the major component of local immunity.
This refers to the overall level of immunity in a community. When a large proportion of individuals in a community(herd)are immune to a pathogen,the herd immunity to the pathogen is satisfactory. Eradication of communicable diseases depends on the development of a high level of herd immunity rather than on the development of a high level of immunity in individuals.